Biopsies | Vibepedia
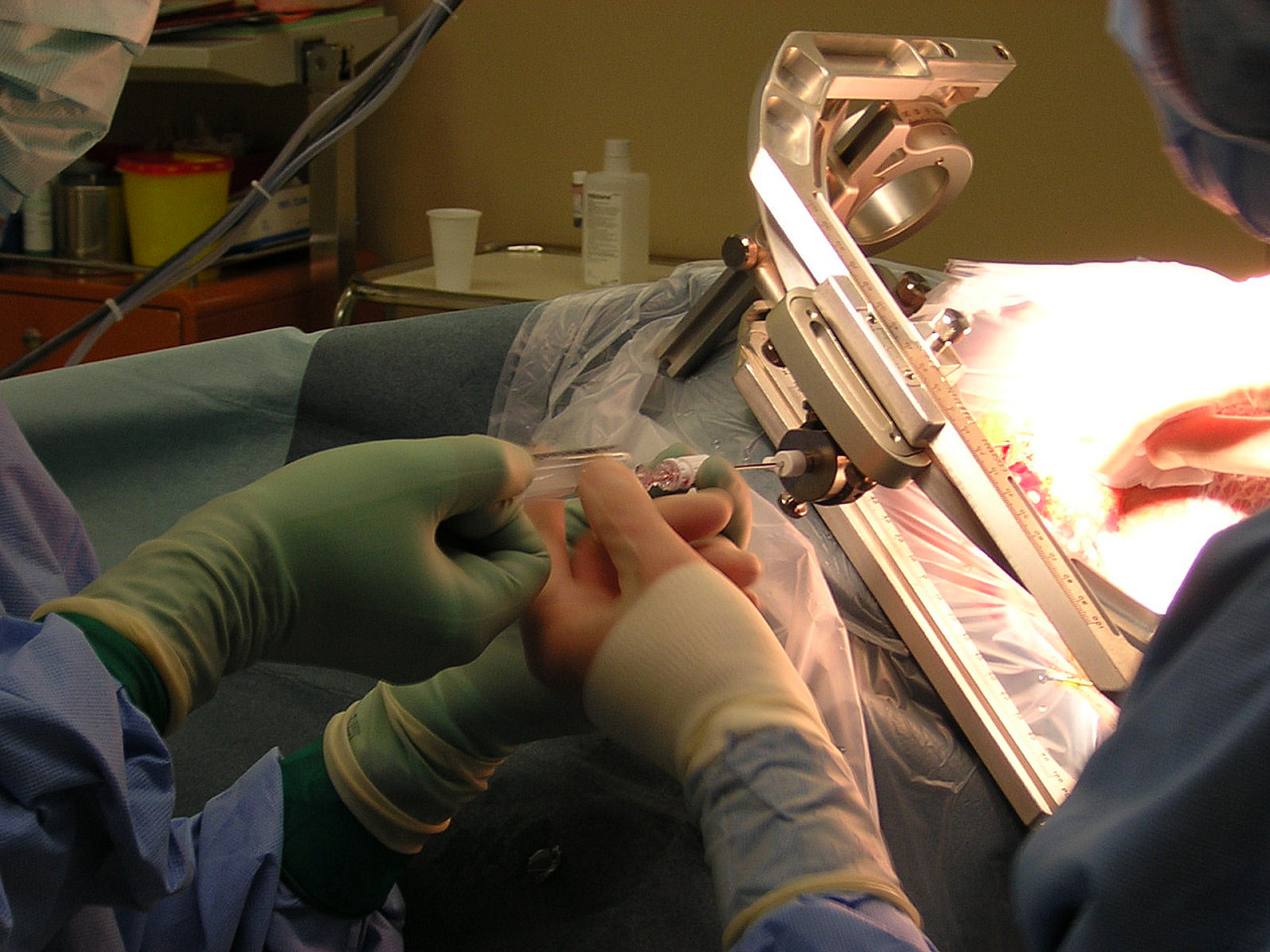
A biopsy is a critical medical procedure involving the extraction of tissue or cells for microscopic examination. This invasive test, performed by various…
Contents
Overview
The concept of examining diseased tissue dates back centuries, with early physicians like Rudolf Virchow in the mid-19th century laying the groundwork for cellular pathology, though the term 'biopsy' itself, derived from Greek 'bios' (life) and 'opsis' (sight), gained traction later. Early biopsies were often crude, relying on macroscopic observation or rudimentary dissection. The development of staining techniques by Paul Ehrlich and others in the late 19th and early 20th centuries revolutionized microscopic analysis, making detailed cellular examination feasible. The establishment of pathology as a distinct medical specialty, championed by figures like William Osler, solidified the biopsy's place in clinical practice.
⚙️ How It Works
The process of performing a biopsy is a multi-stage endeavor, beginning with the extraction of a tissue sample. This can be achieved through various methods: a surgical biopsy involves direct excision, a needle biopsy uses a hollow needle (like a core needle or fine-needle aspiration) to withdraw tissue or cells, and endoscopic biopsies are taken during procedures like colonoscopies or bronchoscopies. Once obtained, the tissue is preserved, typically in formalin, then processed through dehydration, embedding in paraffin wax, and slicing into ultra-thin sections using a microtome. These sections are mounted on glass slides, stained with dyes like Hematoxylin and Eosin (H&E) to highlight cellular structures, and finally examined by a pathologist under a microscope to identify abnormalities such as cancerous cells, inflammation, or infection. Immunohistochemistry and molecular testing can further refine diagnoses by detecting specific proteins or genetic mutations.
📊 Key Facts & Numbers
The turnaround time for biopsy results typically ranges from 24 hours for rapid assessments to several days for more complex analyses, including molecular profiling which is now standard for many lung cancer diagnoses.
👥 Key People & Organizations
Pioneers in cellular pathology like Rudolf Virchow established the foundation for understanding disease at the cellular level. Later, Paul Ehrlich developed crucial staining techniques that enabled detailed microscopic examination. In modern practice, pathologists at institutions like the Mayo Clinic and Johns Hopkins Medicine are central to interpreting biopsy results. Organizations like the College of American Pathologists (CAP) set standards for quality control and accreditation, ensuring the reliability of diagnostic services worldwide. Interventional radiologists, such as those at the Society of Interventional Radiology, are increasingly performing image-guided biopsies, enhancing precision and patient safety.
🌍 Cultural Impact & Influence
Biopsies have profoundly shaped public perception of disease, particularly cancer, transforming it from a mysterious and untreatable affliction into a diagnosable and often manageable condition. The phrase 'getting a biopsy' has entered common parlance, often associated with anxiety and the critical juncture of a medical diagnosis. Media portrayals, from dramatic medical dramas to news reports on celebrity health, frequently feature biopsies as a pivotal plot point, underscoring their perceived importance. Culturally, the biopsy represents a tangible step towards understanding and confronting illness, offering a degree of certainty in the face of uncertainty. The widespread availability of biopsy services has also contributed to increased survival rates for numerous diseases, fostering a societal narrative of medical progress and hope.
⚡ Current State & Latest Developments
The field of biopsies is rapidly evolving, driven by demands for greater accuracy, less invasiveness, and faster results. Liquid biopsies, which analyze circulating tumor DNA (ctDNA) or cells in blood or other bodily fluids, are emerging as a powerful alternative or adjunct to traditional tissue biopsies, particularly for monitoring treatment response and detecting recurrence in cancer patients. Advances in artificial intelligence are being integrated into digital pathology, assisting pathologists in analyzing biopsy slides with enhanced speed and accuracy, potentially identifying subtle patterns missed by the human eye. Robotic-assisted biopsy systems are also being developed to improve precision in hard-to-reach areas, reducing complications and improving sample acquisition. Furthermore, the integration of genomic sequencing directly from biopsy samples is becoming standard for personalized medicine, guiding targeted therapies.
🤔 Controversies & Debates
One persistent controversy revolves around the potential for sampling error in biopsies. Because only a small portion of a tumor or lesion is examined, there's a risk that the sampled tissue may not be representative of the entire abnormality, potentially leading to false negatives or underestimation of disease severity. This is particularly debated in conditions like prostate cancer, where sampling strategies are complex. Another area of contention is the cost and accessibility of advanced biopsy techniques and subsequent molecular testing, raising concerns about healthcare equity. The ethical implications of incidental findings in biopsies, particularly from screening procedures, also spark debate regarding patient notification and management. Furthermore, the increasing reliance on liquid biopsies raises questions about their validation and regulatory approval compared to established tissue-based methods.
🔮 Future Outlook & Predictions
The future of biopsies points towards increasingly non-invasive and intelligent diagnostic tools. Liquid biopsies are expected to become more sophisticated, offering comprehensive genomic profiling from a single blood draw and potentially replacing tissue biopsies for many indications. AI-powered diagnostic platforms will likely become standard, augmenting pathologist capabilities and potentially leading to earlier and more accurate diagnoses. The development of real-time, in-situ biopsy techniques, perhaps using advanced imaging or nanotechnology, could allow for immediate analysis during the procedure, drastically reducing turnaround times. We may also see biopsies integrated more seamlessly with wearable technology for continuous monitoring of disease markers. The ultimate goal is a paradigm shift towards proactive, personalized diagnostics that minimize patient discomfort and maximize therapeutic efficacy.
💡 Practical Applications
Biopsies are indispensable in numerous medical applications. They are the gold standard for diagnosing cancer in virtually all organs, from the skin and breast to the lung and liver. They are crucial for identifying the cause of inflammatory conditions like autoimmune diseases (e.g., kidney biopsies in lupus nephritis) and infectious diseases (e.
Key Facts
- Category
- science
- Type
- topic