Addison's Disease | Vibepedia
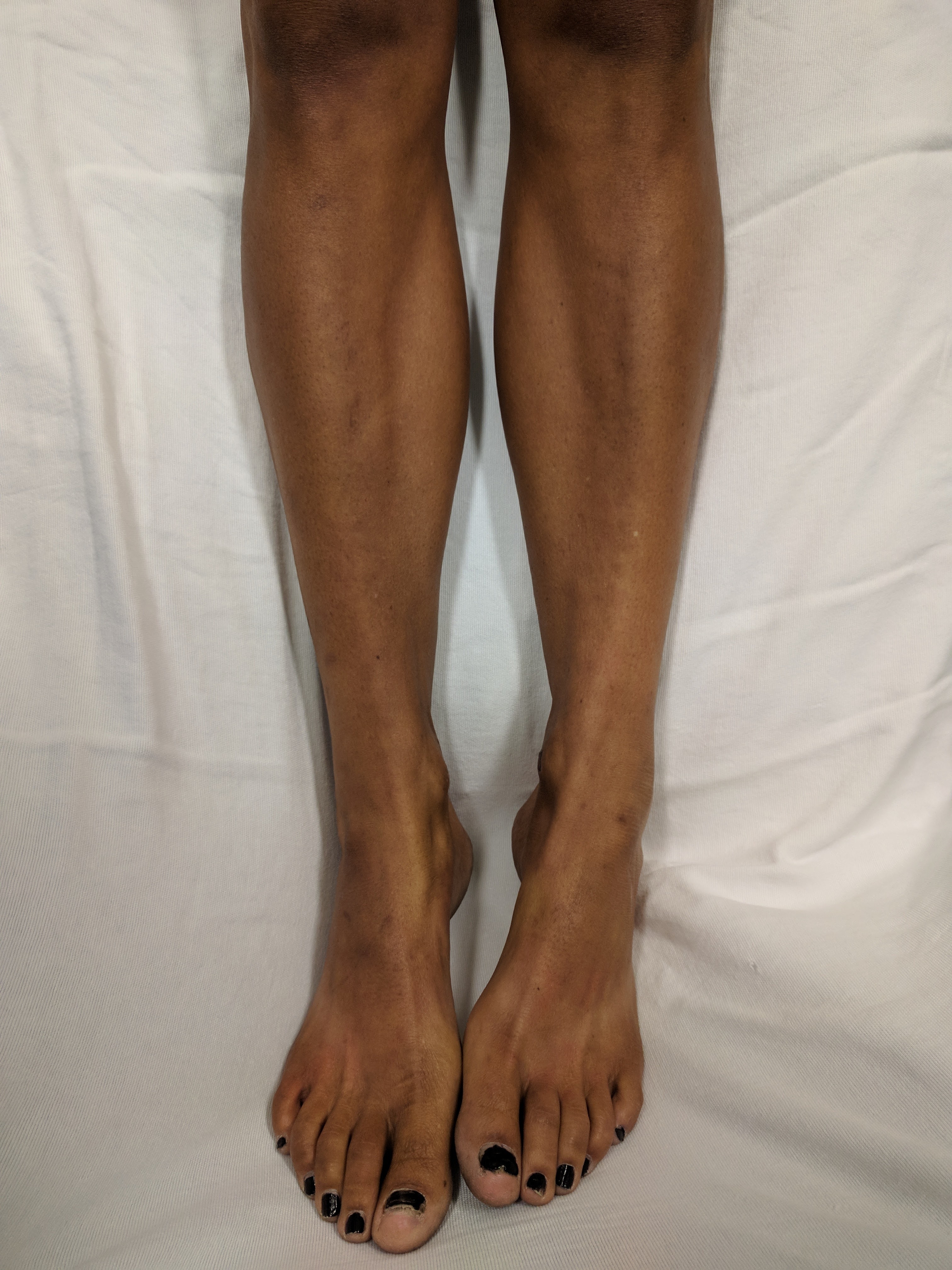
Addison's disease, also known as primary adrenal insufficiency, is a rare but serious autoimmune disorder where the body's own immune system mistakenly…
Contents
Overview
Addison's disease, also known as primary adrenal insufficiency, is a rare but serious autoimmune disorder where the body's own immune system mistakenly attacks and damages the adrenal cortex. This damage leads to an insufficient production of vital steroid hormones, primarily cortisol and aldosterone, which are crucial for regulating metabolism, immune response, blood pressure, and electrolyte balance. The insidious onset of symptoms, often including profound fatigue, unexplained weight loss, muscle weakness, and distinctive skin hyperpigmentation, can make diagnosis challenging. Without timely intervention, individuals are at risk of a life-threatening adrenal crisis, a medical emergency characterized by severe hypotension and shock. While incurable, Addison's disease is manageable with lifelong hormone replacement therapy, fundamentally altering a patient's daily life and requiring constant awareness of potential triggers for exacerbation.
🎵 Origins & History
The story of Addison's disease begins with the meticulous observations of Thomas Addison, an Irish physician. Addison described profound weakness, anemia, gastrointestinal distress, and a characteristic bronzing of the skin in patients with diseased adrenal glands. His groundbreaking monograph, based on post-mortem examinations, was initially met with skepticism by the medical establishment, as the function of the adrenal glands was poorly understood at the time. It wasn't until the early 20th century, with advancements in endocrinology and the isolation of adrenal hormones, that Addison's clinical descriptions were fully validated and the condition was formally named in his honor. Prior to Addison's work, similar symptoms might have been attributed to a variety of vague ailments, but his precise clinical correlations laid the foundation for understanding this specific endocrine failure.
⚙️ How It Works
At its core, Addison's disease represents a failure of the adrenal glands to produce adequate amounts of essential steroid hormones. In primary adrenal insufficiency, the damage is to the adrenal cortex itself, most commonly due to an autoimmune attack where the body's immune system mistakenly targets its own adrenal cells. This autoimmune process, often linked to genetic predispositions and other autoimmune conditions like Type 1 diabetes and thyroid disease, destroys the cells responsible for synthesizing cortisol and aldosterone. Cortisol is vital for stress response, immune function, and regulating blood sugar, while aldosterone controls sodium and potassium balance, impacting blood pressure. Without these hormones, the body struggles to maintain basic physiological functions, leading to the diverse and often debilitating symptoms experienced by patients. Secondary adrenal insufficiency, conversely, stems from insufficient ACTH production by the pituitary gland, which signals the adrenals to produce cortisol, but does not typically affect aldosterone production.
📊 Key Facts & Numbers
Addison's disease affects approximately 1 in 100,000 people worldwide, making it a rare condition. The autoimmune form accounts for about 80-90% of all cases, with tuberculosis being a historical, though now less common, cause in some regions. Diagnosis often occurs between the ages of 30 and 50, with a slight female predominance in autoimmune cases. The risk of developing an adrenal crisis is a significant concern; these life-threatening events can occur with as little as a 50% reduction in cortisol production and are often triggered by physical stress, such as infections, surgery, or trauma. Without prompt treatment with intravenous corticosteroids and fluids, an adrenal crisis can lead to profound hypotension, shock, and death, with mortality rates historically exceeding 50% before modern medical interventions. Lifelong hormone replacement therapy, typically involving hydrocortisone and fludrocortisone, costs an estimated $1,000 to $3,000 per year per patient in the United States, depending on insurance and specific medication regimens.
👥 Key People & Organizations
The foundational figure is undoubtedly Thomas Addison, an Irish physician, whose 1855 publication first described the syndrome. Modern understanding owes much to endocrinologists like William Montague Cann, who conducted early research on adrenal physiology, and Oscar Minkowski, who, along with Josef von Mering, explored the role of the adrenal glands. The Endocrine Society and the Adrenal Foundation are key organizations dedicated to patient support, research funding, and raising awareness for adrenal insufficiency. Pharmaceutical companies such as Novartis and Pfizer are major players in developing and distributing the essential hormone replacement therapies, including hydrocortisone and fludrocortisone, that are critical for managing the condition. Patient advocacy groups, like the National Adrenal Diseases Foundation (NADF), play a crucial role in connecting patients and providing vital resources.
🌍 Cultural Impact & Influence
Culturally, Addison's disease often remains in the shadows, a rare condition rarely depicted in mainstream media. When it does appear, it can sometimes be sensationalized or misunderstood, contributing to public ignorance. The most significant cultural impact is on the lives of affected individuals and their families, who must navigate the daily realities of managing a chronic illness. This includes the constant need for medication, awareness of potential triggers for adrenal crisis, and the psychological toll of living with a potentially life-threatening condition. The distinctive skin hyperpigmentation, a hallmark symptom described by Addison, has sometimes been a source of curiosity or concern for patients, though it is now understood as a direct physiological consequence of the hormonal imbalance. The experience of living with Addison's disease underscores the profound impact that subtle physiological changes can have on one's quality of life and the importance of accessible healthcare.
⚡ Current State & Latest Developments
Current research focuses on improving diagnostic accuracy and developing more sophisticated monitoring tools for patients with Addison's disease. Advances in autoimmune disease research are shedding light on the precise mechanisms driving the adrenal cortex destruction, potentially paving the way for future immunomodulatory therapies that could slow or halt disease progression. There's also ongoing work in developing more convenient and stable hormone replacement formulations, aiming to better mimic the body's natural diurnal cortisol rhythm and reduce the burden of frequent dosing. The development of smart devices for continuous glucose monitoring is inspiring similar explorations for hormone levels, though a practical, widely available continuous cortisol monitor remains a significant challenge. The global health community continues to emphasize the importance of early recognition and management of adrenal insufficiency, particularly in resource-limited settings where diagnostic tools and medications may be less accessible.
🤔 Controversies & Debates
A significant debate revolves around the optimal management of stress and illness in Addison's patients. While the "stress dose" protocol—increasing corticosteroid intake during periods of illness or stress—is standard, the precise guidelines for dosage and duration can vary, leading to potential under- or over-treatment. Some endocrinologists advocate for more aggressive stress dosing, citing the high mortality associated with adrenal crises, while others emphasize the risks of Cushing's syndrome from prolonged high-dose steroid use. Another area of discussion is the role of genetics; while certain HLA genes are strongly associated with autoimmune Addison's, the exact interplay of genetic susceptibility and environmental triggers is still being elucidated. Furthermore, the long-term effects of lifelong hormone replacement therapy on bone health, cardiovascular risk, and metabolic function are subjects of ongoing study and clinical debate.
🔮 Future Outlook & Predictions
The future of Addison's disease management likely lies in personalized medicine and advanced biotechnologies. Gene therapy or targeted immunotherapies could potentially offer a cure by restoring adrenal function or preventing the autoimmune attack altogether, though these are still distant prospects. Research into bioengineered adrenal tissues or advanced drug delivery systems, such as long-acting injectable corticosteroids, could significantly improve patient convenience and adherence. The development of wearable biosensors capable of real-time hormone monitoring would empower patients and clinicians with more precise data, allowing for proactive adjustments to therapy and potentially preventing adrenal crises. Experts predict that within the next 10-15 years, we may see the emergence of more sophisticated diagnostic tools that can identify individuals at high risk for developing Ad
Key Facts
- Category
- science
- Type
- topic